 To say that amputees have phantom limbs and whole-bodied people do not is misleading. The so-called ‘phantom’ is the brain’s representation of the body, something everybody has. As neurologist Ronald Melzack put it, “the phantom represents our normal experience of the body.” [Melzack, 1989, p 4]
To say that amputees have phantom limbs and whole-bodied people do not is misleading. The so-called ‘phantom’ is the brain’s representation of the body, something everybody has. As neurologist Ronald Melzack put it, “the phantom represents our normal experience of the body.” [Melzack, 1989, p 4]
Amputees differ from other people in that they notice their phantom limbs, while the rest of us do not. They notice them because the corresponding limb of flesh and blood is missing. The difference between representation and reality is what makes the amputee’s phantom salient. The rest of us fail to notice our body phantoms because, when all is well, we cannot distinguish them from our bodies themselves.
I have started to think of the phantom as ‘the brain’s user interface to the body.’ It’s a very good interface, one that might have been designed by a genius like Steve Jobs. It gives your brain exquisite control over your body while remaining utterly transparent to you, the user. Most people go through life without ever realizing that the interface exists.
The interface is so transparent, it only becomes visible at all when there are discrepancies between representation and reality. In this blog, I’ve taken brief looks at two kinds of discrepancy: the phantom limbs which almost all amputees experience, and the rubber-hand illusion which allows an ordinary person to observe her phantom from a new perspective by tricking her brain into shifting the phantom from her real hand to an obviously fake, dummy hand.
BIID: A Discrepancy Between Body and Phantom?
While researching discrepancies between body and phantom in greater depth for a book in progress, I grew interested in Body Integrity Identity Disorder (BIID). This remarkable condition, which non-afflicted people find very hard to understand, is characterized by an intense desire to amputate a healthy arm or leg. How could any sane person want to be rid of a perfectly good limb, which serves them well in all the business of life? Yet there are people who have this very specific desire, and although not common, it is not all that rare; numerous BIID studies draw on clinical information from 10-50 subjects, and some internet groups for people with BIID have over 1000 members. It is a serious condition. BIID is often a lifetime affliction, a source of unhappiness strong enough to motivate many to carry through with the desired amputation against all obstacles. Unable to find a surgeon willing to cooperate, they resort to such drastic, dangerous, and excruciating tactics as blasting a leg with a shotgun, crushing it under a train, or freezing it with dry ice, with the aim of damaging it to the point that amputation becomes medically necessary.
BIID has other names, which emphasize different aspects of the disorder. One that is increasingly preferred by researchers is “xenomelia,” from the Greek for “foreign limb.” The term draws attention to the subject’s strong feeling that the limb in question does not ‘belong’ to him in the way that other parts of his body belong. It is ‘intrusive,’ not part of the person himself. He does not have the sense of ‘ownership’ he has for the rest of his body. He may feel that the limb is ‘over-present.’ Asked to describe his leg, one man said, “My soul doesn’t extend into it.” [Guardian, 2012] The feeling must be very uncomfortable, and is certainly a source of enduring unhappiness and a nagging desire for change.
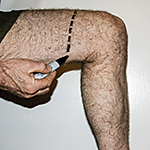
Amputation desire typically begins as far back in childhood as sufferers can remember. More men than women are affected. The limb is more often a leg than an arm, more often on the left than the right. Sometimes bilateral amputation is desired. People with BIID often know exactly where to cut; they can draw a precise line of demarcation between the ‘foreign’ part of their affected limb and the part that feels like their own body. In those cases, the amputation desire is stable as well as specific; it is always for the same leg, always the same line of demarcation. Usually, if a leg, it is above the knee; if an arm, below the elbow. [First, 2005]
Remarkably, when subjects succeed in obtaining an amputation at the desired site, their unhappiness is almost always resolved! Even though they must adapt to living with a disability, learning to use a prosthesis, coping with wheelchairs, realizing the inevitable difficulties and limitations of life in a world that is far from fully accessible to the handicapped, they report lasting feelings of wholeness, satisfaction, and happiness. The amputation solved a problem for which they could find no other cure.
Here are two testimonials excerpted from several reported by Noll and Kasten (2013):
After more than 7 years as a [left above-knee] amputee, I’m still extremely happy and content with my amputation and my stump! I can’t imagine NOT being an amputee. I feel as though my body is now in tune with my mind! I do not regret my choice to get an amputation at all. Yes, there are times where it is and can be a challenge, it’s still better than all the suffering I lived through until I got my amputation. I love waking up and seeing my stump there.
And:
Everything needs more time and is more tiresome. I can’t do everything, what I’ve done before, especially (at least currently) mountain-walking, bicycle-riding, volleyball, and so on. In addition working in the garden is not as easy as before, e.g. to mow the lawn on a hill is impossible for me. All these things my woman has to do now. I must learn to walk with a prosthesis, this was difficult and tedious. Walking outside still needs (currently) absolute concentration and attention, especially when the ground makes it necessary and due to this I have problems to recognize the environment as good as earlier. Going on stairs is tiresome and my radius is restricted. I needed a lot of time for physiotherapy and walking-school. But all these disadvantages are stepping into the background in contrast to the advantages, what means I take them into account to have reached the great goal.
An older term for BIID is “apotemnophilia,” which emphasizes the desire for amputation. This is often interpreted as sexual desire—and, indeed, there is a sexual component to many BIID cases, but by no means all. Such cases are more likely to be of later onset (near puberty), and less likely to be stable and specific with respect to the affected limb and precise line of demarcation. Some of these subjects are sexually drawn to amputees. People who want amputations are not all alike; variations cover a range wide enough that at least one researcher, Michael First, recommends classifying the disorder as a spectrum covering three major groups, designated by the three names under discussion. The groups overlap, many subjects reporting symptoms characteristic of two, or sometimes all three of them. [First, 2005] In order to understand the causes of amputation desire, it is important to begin by determining each subject’s place in this spectrum of symptoms.
For insight into the human body-phantom, the cases of most interest are the ones First classifies as “BIID.” These are characterized by early childhood onset (suggesting congenital origin), stability and specificity (the affected limb never changes, and there is a precise line of demarcation), and the fact that the subject’s primary motive for wanting an amputation is to “correct a mismatch between the person’s anatomy and sense of his or her ‘true’ self (identity).” [First, 2005] It is on those cases I will focus in this post.
The Negative Phantom Hypothesis
One theory of BIID is that it is the inverse of the amputee’s phantom limb. Instead of a phantom without a limb, it is a limb without a phantom. [Ramachandran and McGeoch, 2008, Hilti and Brugger, 2010, Hilti et al 2013 ] The amputee retains a complete internal representation of his or her limb after the limb has been removed; the phantom is complete, but the body is not. A person with BIID, on the other hand, has a complete physical limb but an incomplete phantom. This gives rise to the feeling that the body part not represented in the brain is foreign; it doesn’t ‘belong.’
There is an even closer symmetry between BIID sufferers and people who are born missing one or more limbs, but who have phantoms that persist into childhood, at least long enough for them to notice and talk about them. A child with this condition (dysmelia) has a phantom leg, but never had a real leg. The BIID child, who has a real leg, seems to be missing the internal representation of the leg. This child has an incomplete body representation, a ‘negative phantom.’
Although the idea is appealing, the ‘negative phantom’ explanation of BIID is hard to reconcile with facts: (1) People with BIID receive normal, or close to normal, sensory input from their affected limbs. Their subjective experience of the disowned limb comes pretty close to Melzack’s description of the phantom as the “normal experience of the body”—except for the feeling of alienation. (2) They have normal, or close to normal, motor control over those limbs. There is some evidence that the body-phantom plays an important role in motor control. Dr. Michael Kremer wrote, “I am quite certain that no amputee with an artificial lower limb can walk on it satisfactorily until the body-image, in other words the phantom, is incorporated into it.” [Sacks, 1985, p64] (3) More glaring evidence against the negative phantom hypothesis is the fact that most people with BIID who succeed in having amputations also experience phantom limb sensations afterwards. In a survey of 18 post-amp BIID patients conducted by Kasten and Noll, 17 reported “sensations in their phantom limbs,” including phantom limb pain. [Kasten and Noll, 2013; confirmed by Kasten in private correspondence, Nov 2013] This is close to the incidence of phantom-limb phenomena found in the general population of amputees.
The negative phantom limb hypothesis also raises a deeper question. The human body-phantom is well known to be plastic. The rubber-hand illusion (described below) demonstrates that the phantom will ‘invade’ a suitable target, if supported by synchronized visual and tactile input. Someone with BIID also experiences synchronized visual and tactile sensations when his ‘disowned’ leg is touched, raising the question why his phantom would not conform to the leg as easily and exactly as it does to the rest of his limbs. To sustain the hypothesis, we must conjecture that the phantom is congenitally incomplete—that part of the brain’s representation of the body is wholly absent—and that the phantom is not sufficiently plastic as to restore a missing part of itself, even into the ideal target, a living limb.
The Layered-Phantom Hypothesis
Despite these difficulties, there may be something right in the negative phantom idea. To someone with BIID, his disowned limb feels ‘foreign,’ ‘over-present,’ and ‘not part of himself.’ These characteristics suggest a variant of the negative phantom hypothesis. The phantom itself may not be entirely unified. Perhaps multiple ‘phantoms’ represent different aspects of the human body, but because the brain represents them as spatially coinciding with each other (and with the body itself) they are subjectively experienced as a single, unified entity. Perhaps the human body-phantom is best thought of as being composed of distinct layers with different properties and functions. We know the human brain is host to multiple body-maps, instantiated in different areas. There are the primary somatosensory and motor cortices, S1 and M1 (the famous ‘Penfield homunculi’), the secondary somatosensory and motor cortices (S2 and M2), and several others. Each separately instantiated body-map makes an independent contribution to the unified body-experience—Melzack’s ‘phantom’—which the brain presents to the conscious mind.
But if the human body-phantom is composed of distinct layers, how can a person’s ‘normal experience of her body’ be as unified as it is?
The analogy of man-made user interface offers a clue. Software packages that work with images, from Photoshop to PowerPoint to Google maps, use a layering strategy to combine partial images into the final image presented on the user’s screen. Layering affords flexibility, allowing image components to be added, removed, or temporarily hidden to show what lies ‘beneath.’ Images can be rendered semi-transparent, so that the user sees one through another. Layers also allow different underlying technologies, such as vector and bitmap graphics, to be visually combined while retaining their independent advantages; the edges of vector graphics remains sharp even when you enlarge the overall image, and you can continue to edit your text.
I suggest that the brain uses a layering strategy to create a unified representation of the body for subjective presentation to the ‘user.’ Within a single three-dimensional spatial coordinate system, it builds the combined ‘phantom’ out of map-like layers with different content (sensory, motor, affective, perhaps more), which are physically instantiated in different brain areas.
Although this conjecture is highly speculative, it could be supported by the same kind of evidence that made the phantom accessible to scientific observation in the first place. Just as the discrepancy between an amputee’s physical body and its representation in his brain made the phantom ‘visible,’ discrepancies between different layers of the phantom may be expected to make those layers visible as distinct entities. When all layers of the phantom coincide perfectly, the phantom appears perfectly unified to its owner. But if there are discrepancies between the layers—if one layer is, for example, missing part of an arm which is present in all the other layers—the person will subjectively experience a difference between his two arms, one that reflects the contribution of that layer to the combined phantom.
Again, the analogy of layered images may be helpful in understanding this. If you look at a composite image in Photoshop, you cannot distinguish the layers it is composed of; but when you ‘hide’ layers, making them temporarily invisible, you can see what contribution each one makes to the final image.
BIID could be symptomatic of a discrepancy of this nature. If one layer of the brain’s internal body-representation were responsible for a person’s sense of ‘ownership’ of his own body, and if that layer were incomplete—missing part of an arm or leg—the effect might be the antipathy towards a specific body-part we see in BIID.
A Layered-Phantom Explanation of BIID?
If the motor and somatosensory components of the human body phantom are distinct layers, then perhaps another layer contains the emotional component—the affective dispositions and feelings that people normally have for their own bodies. This layer may include protective feelings of body ‘ownership.’ These feelings are subjectively located in space; they are felt in specific parts of the body. Just as sensations of touch, itchiness, and pain are felt in the body, ‘ownership’ of my hand is something I feel in my hand. It is the feeling that someone might describe in terms such as, “My hand belongs to me,” or, “My soul extends into it.”
BIID, I suggest, may be caused by a discrepancy between the affective ‘ownership’ layer and the other layers of the body phantom. The somatosensory and motor layers of someone with BIID are mapped to the body accurately, but the affective layer fails to represent the portion of the disowned limb distal to the line of demarcation.. Since that layer is responsible for the sense of bodily ownership, this would explain why someone with BIID has the bizarre experience of controlling the movements of a leg, feeling sensations in its skin and contact with everything it touches, but also feeling that it is not his leg.
The stability and early onset of BIID, and the precise line of demarcation, further suggest the condition is congenital. People in this part of the BIID spectrum are born missing the representation of an arm or leg in their affective body-map.
The Rubber-Hand Illusion: More Evidence for a Layered Phantom
Corroborating evidence that the human body phantom has an affective component that can become dissociated from somatosensory components is found in Tsakiris’s (2010) work on the rubber-hand illusion.
The rubber-hand illusion is a popular science-fair demonstration of plasticity in the human body-phantom. Typically, the experimental subject is asked to sit with both hands extended on the tabletop in front of her. A screen is placed so as to block her view of one hand, and a dummy hand is put on the table where she can see it. If the left hand is hidden, a left-hand dummy is used, but in other respects, the dummy need not be very realistic. A rubber glove stuffed with dried lentils will work, as I can attest from a home experiment. The dummy hand should be oriented in the same direction as the real hand. It need not be connected to anything at all, but the illusion may be easier to induce if the dummy has a rough facsimile of a forearm (such as a rolled newspaper under a cloth) extending towards the subject’s body. None of this setup is hidden from the experimental subject, who knows exactly what’s going on.
The subject is asked to watch while the experimenter taps and strokes the dummy hand with a finger, stylus, or small brush. The experimenter also taps and strokes corresponding points of subject’s real hand behind the screen, in synchrony with the taps and strokes to the dummy hand. After some time (usually 2-15 minutes , although the effect has been recorded in as little as 12-15 seconds), the subject begins to feel the taps and strokes in the dummy hand!
The illusion is an eery experience. ‘Illusion’ does not imply that the subject is deceived, any more than ‘optical illusion’ carries that implication; in fact, its eeriness depends on the dissonance between what the subject knows—that her real hand is behind the screen, and she is watching a completely unconvincing dummy—and what she feels— that the dummy hand is her own hand.
When the illusion takes hold, the subject will react protectively to a physical threat to the dummy. If, for example, the experimenter suddenly swings a mallet down onto the dummy, the subject flinches, pulling her real hand back. (The subject may also scream when this happens, but will not be genuinely alarmed, because she knows her real hand is safe.) The threat also produces involuntary sweating in the real hand, a measurable Skin Conductance Response (SCR). (Another objective sign that the real hand is no longer ‘occupied’ by the phantom is a drop in its temperature.)
I said the dummy hand need not be realistic. Armel and Ramachandran (2003) found that the illusion can be induced using a shoe instead, or even a bare tabletop. SCR’s are, however, significantly weaker when the form of the target object is not hand-like. Tsakiris (2010) argues that they are weaker because the illusion has not fully taken hold. If the target is a tabletop, the subject will have the sense that the taps and strokes she feels are in the tabletop, but she will not feel that the tabletop is part of her body. If the target is anatomically unlike a hand, somatosensory aspects of the phantom invade it, but the affective aspects—the sense of body ownership, the protective responses when the target is endangered—do not. Only if the dummy is hand-like in form does the subject develop the warm, familiar and protective attitude she has towards the rest of her body.
On the layered phantom hypothesis, the weaker illusion induced in the tabletop or the shoe can be explained as displacement of some, but not all, layers of the body-phantom to the space occupied by the target object. Although the somatosensory layer invades the space of the tabletop, the affective layer responsible for the sense of body ownership does not.
What Explains the Amputation Desire?
If BIID can be explained as lack of representation of a body part in the ‘ownership’ layer of the phantom, an important question remains. Why does someone with BIID have such a deeply disturbing experience of his unwanted limb—unpleasant enough to motivate the drastic remedy of self-amputation? Why such revulsion towards it, instead of indifference?
Ramachandran, in arguing for a version of the ‘negative phantom’ hypothesis, attributes amputation desire to “mismatch aversion.”
Lack of coherence, or mismatch, between the outputs of brain modules can create alienation, discomfort, delusion, or paranoia. The brain abhors internal anomalies—such as the mismatch between emotion and identification in Capgras syndrome—and will often go to absurd lengths to deny them or explain them away. (I emphasize “internal” because generally speaking, the brain is more tolerant of anomalies in the external world. …) [Ramachandran, 2011, pp 256-257]
People with BIID have normal (or almost normal) somatosensory input from their disowned limbs, but do not feel that the limbs are theirs. This mismatch, or discrepancy, creates a nagging problem for the brain, which it tries to solve by amputation.
This answer is unpromising, for the same reasons the negative phantom hypothesis doesn’t work. Amputation does solve the problem for people with BIID; in giving them the body shape they feel is right, it cures their unhappiness. Yet most BIID amputees continue to have somatosensory sensations in phantom limbs. That mismatch persists even after amputation; but it is no longer distressing.
People with BIID are not delusional; they have accurate cognitive models of their own bodies. Although they may have phantom sensations that seem to originate in the amputated limbs, they are perfectly well aware that the amputation took place. And that is enough to relieve their distress. Their bodies feel the right shape, with no superfluous parts. A discrepancy has been resolved, but not a simple discrepancy between the phantom as a whole and the body. What has changed is that the cognitive representation of the body now matches the affective representation of the body as it should be—what I’ve called the ‘ownership layer.’
The word “ownership” doesn’t adequately describe the motivational force with which this layer is imbued. My attitude towards my body carries much more emotional weight than my attitude towards other things I own. In recognizing my arm as part of me, I include it within the sphere of my self-concern. Most people are fiercely protective of everything within that sphere.
If the ‘disowned’ limb of someone with BIID is not represented in the ‘ownership’ layer of the phantom, it might feel subjectively like an alien thing that has intruded into the inner sanctum of the self, one’s own body. That would be alarming, like learning that someone in one’s most trusted circle is a mole. Only parts of one’s self belong in one’s body, anything else—a bullet, a cancer—is invasive and potentially dangerous.
But this is a partial explanation at best of the desire that people with BIID have to rid themselves of their disowned limbs. People do accept some ‘alien’ things into their bodies—transplanted kidneys and titanium knees for example. Even if I didn’t feel that my arm belonged to me, why wouldn’t I accept and use it as a tool that comes to hand? Why wouldn’t I be grateful for the value it offers, without needing to feel that it is part of myself?
The strong aversion felt by people with BIID towards their disowned parts cries out for further investigation. One promising direction lies in comparing BIID to other conditions in which people reject or disown parts of their own bodies: conditions including transsexuality, Body Dysmorphic Disorder (BDD), and somatoparaphrenia, a syndrome of stroke victims who deny that their paralyzed limbs belong to them . Another approach is to systematically explore the neurological underpinnings of these conditions and other ‘phantom discrepancies’ such as the rubber hand Illusion. Recent research in this field has been extremely active.
The Neurology of BIID
One brain area of great interest is the Superior Parietal Lobule (SPL). Ramachandran (2011) describes it as an place where information from several body maps, including the primary and secondary somatosensory cortices (S1 and S2) are combined, along with visual input and vestibular information from the inner ear, into “a unified, real-time representation of your physical self.” [Ramachandran, 2011, p 256] His associates McGeoch and Brang concur, calling the SPL in the right brain hemisphere (rSPL) “a cortical area that appears ideally placed to unify disparate sensory inputs to create a coherent sense of having a body.” [McGeoch et al, 2011, p 1314]
Using magnetoencephalography, McGeoch et al (2011) measured the rSPL’s response to tactile stimulation on various parts of the body in male subjects with BIID and in normal controls. In the four subjects with BIID, the authors found significantly reduced rSPL response when their affected limbs were touched, compared to the unaffected limbs of the same subjects and those of normal control subjects. They reported a positive correlation between the amount of this reduction and the subjects’ self-reported intensity of their desire to amputate. No such difference in response was found in neighboring brain areas.
The weak rSPL response when the disowned body part is touched suggests that this brain area may be responsible for generating the sense of body ownership. If there is an ‘ownership layer’ to the body phantom, then perhaps the rSPL is home to it, or closely connected.
Damage to the rSPL can cause people to lose their sense of body ownership. Some stroke patients with paralysis of a left arm or leg deny the paralysis, and some of those deny that the paralyzed limb is their own—a condition called somatoparaphrenia. They may believe that the inert limb in their bed belongs to someone else, such as their doctor or a relative. They usually feel aversion towards the disowned limb; patients are frequently horrified to wake up and find what they believe to be someone else’s leg in their bed. Unlike people with BIID, these patients are delusional. But they are not psychotic; their delusion is a very specific one. In these cases, stroke damage to the rSPL is invariably found. [Ramachandran, 2011, pp 258-259]
The sense of ‘owning’ one’s body is an emotional attitude. To understand its neurology, we need to understand how it is connected to the motivational centres of the brain. The insula, which is connected both to the SPL and to the amygdala—a mid-brain structure that orchestrates parasympathetic responses to emotionally-laden stimuli, and is central to our emotional life—may play a role in this. [Brang et al, 2008]
The insula mediates Skin Conductance Responses, a recognized measure of emotional arousal. When people with BIID are pricked on the skin below the line of demarcation on their disowned limbs, their SCR’s are significantly (2-3 times) higher than when they are pricked above the line or on unaffected limbs. [Brang et al, 2008, McGeoch 2009] Brang et al (2008) offer a ‘mismatch’ explanation of the heightened SCR. The pin-prick to the disowned area is a highly salient reminder to the brain that it is receiving somatosensory input from a body part that is not represented as part of the person’s own body—an alarming incongruence which activates the insula.
More research is needed before we can draw conclusions about the exact mechanisms by which the brain produces the desire to amputate a healthy body part. But impressive progress has been made, and I have no doubt that, within a few years, it will yield a picture of BIID which not only explains that surprising disorder, but sheds new light on how normal people tick—on the functional role of emotions concerned with their own bodies.
Body Identity and Gender Identity
Some light has already been shed. BIID research done so far strongly suggests the existence of an inner representation of the body with which people closely identify—a representation that defines what they feel to be themselves. Any discrepancy between this representation and the actual body is disturbing to the individual. Not only is it disturbing, it creates a desire to make the body conform to the inner representation, not the other way around.
Evidence of this is seen not only in BIID, but in the better-known phenomenon often labelled Gender Identity Disorder (GID) in clinical literature, but for which I will use the more widely-accepted term, “transsexuality.” Like people with BIID, transsexuals are born with bodies that do not fit their brains’ images of themselves. They too desire to reshape their bodies to conform to the image they take to represent their true selves. They are willing to undergo extensive surgery, including breast or penis amputations. To achieve their goals, they are often willing to accept some impairment of bodily function—specifically, reproductive function.
Laura Case argues compellingly for a common explanation of transsexuality and BIID in terms of body image. Like BIID, transsexuality is a discrepancy between the body and an internal representation of the body. Transsexuals experience their ‘incongruent’ body parts as “over-present” and aversive; they also show heightened SCR’s when those parts are touched, compared to other parts of their bodies. [Case, 2013, ch 1]
As in BIID, there is little or no discrepancy between a transsexual’s body and his or her somatosensory experience. The breasts of a female-to-male transsexual (before surgery) have more-or-less normal sensitivity to touch, as does the penis of a male-to-female transsexual. What does not match is the sense of the true self. Transsexuals typically say they feel like “a man trapped in a woman’s body,” or the converse.
Transsexuals who have not yet undergone sex-reassignment surgery may experience phantom body parts of the opposite sex.[Ramachandran, 2008] (This has no parallel in BIID, where the desire is always to remove body parts, never to add them.) After surgery, transsexuals sometimes experience phantom sensations of the amputated breasts or male genitalia, but their incidence is significantly lower than when the same parts of non-transsexual persons are amputated. [Ramachandran, 2008]
A phantom penis, experienced by someone who has always been anatomically female, suggests that transsexuality is caused by an internal body image which is of the opposite sex to the body itself. Even so, exceptions in both directions (presurgical transsexuals who do not experience such phantoms, and post-surgical ones who report phantoms of the ‘incongruous’ parts that were removed) remain to be explained. Perhaps the answer will be found in discrepancies within the phantom itself. If the body-phantom is composed of layered body maps with different functions, then transsexuals may have layers that do not agree in their representation of sexual anatomy. If the somatosensory layer has breasts, and the ‘ownership layer’ has a penis, then perhaps the same female-to-male transsexual individual could experience phantom sensations of a penis before sex reassignment surgery, and of breasts afterwards. Discrepancies between layers could produce weak or confused phantom sensations, and account for the lack of unanimity in phantom reports in both BIID and transgender groups.
Transsexuals and people with BIID both have the strong, persistent feeling that their ‘true selves’ are anatomically different from their bodies. Both have internal representations of their bodies that, they feel, represent them as they ‘really are’. Both feel alienated from parts of their actual bodies that do not fit the body-image with which they most closely identify, and both are motivated to reshape the body to fit the internal image. In order to do so, they are willing to undergo pain, expense, and (in the case of BIID at least) physical impairment.
The other way of resolving the discrepancy—reshaping the body-image to match the body—is rarely a topic of discussion. One reason it is not is that nobody knows how to do this (yet). The BIID and transsexual equivalents of the ‘mirror trick’ discovered by Ramachandran, that effectively relieves pain and paralysis in the phantom limbs of amputees, have not been discovered. If they had been, I can’t help wondering whether many people in either group would be interested. The transformational desire is strongly unidirectional.
The ‘Me’ Layer
That the brain supports several different body maps with different functions—somatosensory, motor, and perhaps others—is not controversial. That content from these semi-independent maps is combined into a unified three-dimensional presentation of the organism’s body to itself also seems beyond dispute, since that is, in fact, our normal subjective experience of our bodies. That one of those maps has an affective function, and is responsible for the sense of body ownership, the affectionate and protective attitude that most people have towards their own bodies, remains speculative—suggested, but not proven, by the experiences reported by transsexuals and people with BIID. Proof will have to wait upon a thorough scientific inventory of the neural correlates of those experiences.
If the affective body-map exists, it deserves to be called the ‘me-layer’ of the phantom, because it is so tightly bound to first-person judgements of personal identity. Any part of the body not represented in the map is categorized as “not part of me.” People who experience such discrepancies never say that their sense of body-ownership is not accurate; that their ‘souls,’ which do not match their bodies, therefore misrepresent themselves. When body and ‘self’ disagree, ‘self’ is always right.
Assuming that the phantom does have a ‘me-layer,’ it has the following characteristics:
- It resembles somatosensory and motor layers in being a spatially-organized representation (a map) of the current state of the body.
- It differs from somatosensory and motor layers in its content, which is primarily emotional. Its content includes the protective, nurturing attitude that animals normally have towards their own bodies.
- It explains the sense of body ‘ownership’ that is felt when the body coincides with the affective body-image, and the opposite feeling of alienation towards unrepresented body parts apparent in cases of BIID, transsexuality, and somatoparaphrenia.
- When there are discrepancies between it and other layers of the phantom, or the body itself, the ‘me-layer’ is subjectively preferred as a representation of the ‘true’ self. This preference is typically uncritical, untempered by doubts, even when family, friends, and doctors express shock and bewilderment.
- When there are such discrepancies, the subject invariably desires to reshape the body to match the ‘me-layer’ of the phantom, rather than the other way around.
References
Aoyama et al (2012) “Impaired Spatial-Temporal Integration of Touch in Xenomelia (Body Integrity Identity Disorder)” Spatial Cognition and Computation: An Interdisciplinary Journal, 12:2-3, 96-110
Armel, K, and Ramachandran, V (2003) “Projecting sensations to external objects: evidence from skin conductance response,” Proceedings of the Royal Society B: Biological Sciences, 270.
Brang D, McGeoch PD, Ramachandran VS (2008) “Apotemnophilia: a neurological disorder,” Neuroreport 19:1305–1306.
Case, Laura (2013) How the Body Can Feel Wrong: Sensory Processing and Neural Body Representation in Transsexuality and Anorexia Nervosa. Doctoral dissertation in Psychology and Cognitive Scient at University of California, San Diego.
First, M. B. (2005). “Desire for amputation of a limb: Paraphilia, psychosis, or a new type of identity disorder.” Psychological Medicine, 35(6), 919-928.
Guardian, The (14 Nov 2012) “Please amputate this leg: it’s not mine,” at http://www.theguardian.com/science/2012/nov/14/please-amputate-this-leg, referenced 27 Nov 2013.
Hilti, L et al (2013) “The desire for healthy limb amputation: structural brain correlates and clinical features of xenomelia.” Brain 2013: 136.
Hilti, LM and Brugger P. (2010) “Incarnation and animation: physical versus representational deficits of body integrity.” Exp Brain Res 2010; 204: 315–26.
Kasten, Erich and Noll, Sarah (2013) “Xenomelia left behind: how amputation changed the life of ‘successful wannabes’.” Slideshow from Xenomelia conference held at University Hospital Zurich, 14 Mar – 15 Mar 2013, at http://www.fortbildung.usz.ch/pdf/FS2013/2013_03_14-15_xenomelie.pdf, referenced 13 Nov 2013.
McGeoch, P et al (2009) “Apotemnophilia – the Neurological Basis of a ‘Psychological’ Disorder,” natureprecedings.
McGeoch PM*, Brang D*, Song T, Lee R, Huang MX, Ramachandran VS (2011). Xenomelia: a new right parietal lobe syndrome. Journal of Neurology, Neurosurgery, and Psychiatry, 82, 1314-1319. doi:10.1136/jnnp-2011-300224 *Authors contributed equally to this work.
Melzack, Ronald (1989) “Phantom Limbs, the Self and the Brain,” (The D.O. Hebb Memorial Lecture), Canadian Psychology/Psychologie canadienne 30 (1).
Ramachandran VS, McGeoch P (2008) “Phantom penises in transsexuals.” J Conscious Stud 15.
Ramachandran, VS (2011) The Tell-Tale Brain: A Neuroscientist’s Quest For What Makes Us Human, W.W Norton & Company, New York.
Sacks, Oliver (1985) The Man Who Mistook His Wife for a Hat, and Other Clinical Tales, Summit Books, New York.
Tsakiris, Manos, (2010) “My body in the brain: a neurocognitive model of body ownership,” Neuropsychologia, vol. 48, issue 2.
Return to the Phantom Self home page.

Wow! What a fascinating and important article! This is a great contribution to the growing understanding that the image of a separate self does not reflect an objective state of affairs, but to be a kind of adaptive, layered neuro-biological-environmental mechanism. Your examples and hypotheses are clear and powerful! Thank you!
Thanks Gordon
Much clearer than the textbooks! 🙂
theo
Hi there, I found your article very interesting and helpful. I was wondering if you know of any web groups for people experiencing these symptoms. I’ve come to terms that I think I have a problem with xenomelia and want to talk to others experiencing the same thing. Thank you.
This is in incredibly interesting article that I’ve found to be very useful for my research project on BIID. I am wondering whether ‘negative phantom limb’ is potentially caused through early developmental issues, and if this is the case… how would one go about correcting it. I am struggling to understand whether negative phantom limb is a result of an issue with physical parts of the brain or instead with chemical parts (not sure if this is explained scientifically correctly).
Thanks,
Bella